The latest Ageing Europe publication from Eurostat, the statistical office of the European Union, reports that, at the start of 2019, 101.1 million people in the EU had reached the age of 65. This is the equivalent of 20 per cent of the total population. This is only likely to increase, with a projected 29 per cent forecasted for 2050.
One of the key challenges for healthcare professionals is ensuring accurate, quick and affordable diagnosis. The provision of efficient, effective and, crucially, non-invasive treatment will help to keep older people out of hospital, with the added benefit of reducing the expense associated with personal care. The latest developments in smart optical imaging technology are helping towards non-invasive and unobtrusive health monitoring. The Astonish project was established in 2016 to develop exactly this kind of technology for exactly these types of applications.
Formed under the Electronic Components and Systems for European Leadership (ECSEL) joint undertaking, the project received €5.9m in funding, and spanned six countries. Some 25 organisations took part from across the supply chain, from semiconductor manufacturers to clinical centres testing the final application, with the aim to propose innovations to improve the global competitiveness of the European healthcare industry and deliver technologies that are market-ready to help enhance the longer life of European citizens.
A noble quest
One such organisation is Quest Medical Imaging, which produces camera systems for medical applications, ranging from fluorescence imaging to photodynamic therapy. Its Spectrum system is designed for open and minimally invasive image-guided surgery. It includes a multispectral camera which pictures cancer cells and tissue differences that are not visible to the human eye.
The contrast is created using fluorescence imaging – visualising biological structures with fluorescent labelling. The camera images signals in the near-infrared range. Combining the localisation of specific labelling agents with a true colour image of a surgical site can provide useful information during surgery.
Applications in medicine for systems like this include tumour diagnosis. As tumours manifest and grow the cells start to produce new blood vessels in order to feed their metabolic needs. However, some of these vessels can suffer from low perfusion, which can be picked up by a system like the Spectrum.
Richard Meester, CEO of Quest Medical Imaging, commented: ‘Providing surgeons with visual aids to detect cancerous lesions through a real-time imaging platform will improve patient care and get us one step closer to achieving our mission of fighting cancer with light and improving patient outcomes.’
Vision in green
As part of the diagnostic process, a tumour patient is injected with indocyanine green (ICG). This accumulates in blood vessels, but remains for longer in tumour-induced vessels, which is then seen by the multispectral camera.
It is also possible to diagnose liver metastases using this technology in a similar way, while potential future uses include detecting the sentinel lymph node to improve speed and accuracy in finding the lymphatic channel and nodes. This could also result in the surgeon making smaller incisions and speeding up the entire procedure. Once again, this involves injecting a fluorescent tracer such as ICG into the tumour region, which, used alongside the multispectral camera, allows mapping of the tumour drainage lymphatic system, including nodes and veins. A biopsy of the sentinel lymph node can then be taken for cancer staging.
Translating into real-life use cases, the Leiden University Medical Centre (LUMC) in the Netherlands last year saw a team from its Thoracic Surgery and Surgery departments, alongside the Centre for Human Drug Research, remove a lung tumour, which was detected using fluorescence imaging in what was believed to be the first instance in Europe of using this technique on a lung tumour patient. It had previously been successfully applied to patients with ovarian cancer.
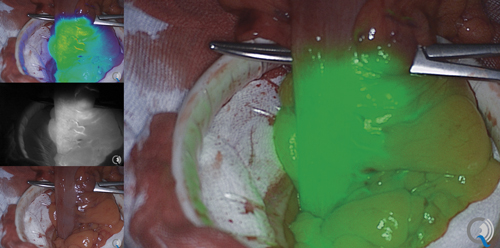
Fluorescence imaging can visualise biological structures with fluorescent labelling. Credit: Quest Medical Imaging
Prior to surgery, the patient was injected with OTL38 – a compound developed by American firm On Target Technologies – consisting of a folic acid-targeting molecule linked to an NIR dye. The compound attaches itself to tumour cells in the body, allowing the surgeon to see the tumour and the possibly affected lymph nodes using Quest’s NIR camera. Dr Jerry Braun, cardio-thoracic surgeon at the LUMC, who co-performed the operation, stated: ‘Identifying the malignant tissue is sometimes difficult. You can’t always see it with the naked eye. You can’t feel it during a viewing operation either.’
Rapid recovery
As well as enabling the identification and removal of malignant tissue, this technology can reduce the chance of discovering, post-surgery, that not all of the tumour tissue has been removed. What’s more, the technique actually helps save tissue, so there is less risk and potentially the patient recovers better.
Braun continued: ‘Metastases are not always visible on a CT scan, especially if they are small or are directly on the pleura. This fluorescence technique is still under development in Leiden and is frequently used in research. The first results with lung surgery are promising. As a result, we can hopefully operate more minimally invasively and with good results.’
Meester added: ‘Adjusting our technology to support OTL38 and participate in a phase three clinical trial is an important step for our Spectrum fluorescence imaging platform.’
Quest also teamed up with biotechnology firm SurgiMab in 2017 in the latter’s development of cancer-specific fluorescent molecules for use in fluorescence-guided oncologic surgery and colorectal cancer (CRC). The partnership formed as SurgiMab was about to begin the phase three clinical trial of its SGM-101 tumour-specific antibody conjugated to a near-infrared fluorochrome.
Phase three is based on compelling results from the company’s phase two study, which saw residual and otherwise invisible tumour tissue detected. The study, which was published in The Lancet Gastroenterology and Hepatology, demonstrated that the use of SGM-101 during surgery can lead to a modification of surgery in 35 per cent of patients with recurrent or peritoneal metastases of CRC, either by allowing more aggressive resection of tumour tissue or by preserving healthy tissue. Quest agreed to provide 12 Spectrum platforms to those medical centres participating in the trial.
Clinical trials
Phase three was designed after discussions with the US Food and Drug Administration (FDA), alongside other regulators. The trial aims to enrol 300 CRC patients in 10 clinical centres across Europe and the US to assess the safety and clinical benefit of using fluorescence-guided surgery with SGM-101 as an intraoperative imaging agent to better identify cancer lesions during the surgical procedure. Patients are injected with 10mg of SGM-101 four days prior to the scheduled CRC surgical procedure.
Vision technology for healthcare applications requires highly precise processes. Credit: Berliner Glas
The first US patient has recently been recruited into this important phase, with four US facilities currently taking part, including: Cleveland Clinic Florida, Massachusetts General Hospital, Moores Cancer Center and the Abramson Cancer Center of the University of Pennsylvania.
Meester said: ‘We are excited to move forward to phase three in order to prove the utility of image-guided surgery, specifically in CRC surgery, which is the third most common type of cancer, affecting people all over the world.’
SurgiMab is optimistic about the results of this next phase, as expressed by CEO Dr Françoise Cailler: ‘If this trial successfully demonstrates that the use of SGM-101 improves tumour resection, we believe that this could provide a new approach for close to 150,000 patients diagnosed with CRC every year in the United States, most of whom undergo surgery.’ Preliminary data is expected next year.
Rise to the challenge
One of the challenges for manufacturers of vision technology for healthcare is just how precise the manufacturing process needs to be. Dr Stefan Beyer, director of product development, medical applications business unit at Berliner Glas, explained: ‘No other industry requires such precise manufacturing processes. In order to make the best possible use of light as a tool with all its fascinating properties, it requires thinking in the dimensions of light and lower. Furthermore, optical applications are not limited to the range of visible light, with wavelengths between 400nm and 700nm; they include the entire spectrum from extreme ultraviolet to far infrared.’
Products for which these highly precise processes are necessary, said Beyer, include optical lens systems or multi-chip modules like those installed in high-quality medical cameras. ‘The multi-chip prism assembly, for example,’ he said, ‘which is used in endoscopic cameras, among other things, is tasked with splitting light into its spectral components, capturing a high-quality image via individual sensors, and merging them again electronically. With resolutions increasing – from HD to 4k to 8k – pixel sizes decreasing accordingly, and data volumes growing, the requirements to adjust sensors to the pixel are increasing to the same degree.’
In fact, stated Beyer, in the area of optics and precision engineering, everything on the spectrum smaller than 10µm is considered a demanding positioning task. ‘In optical systems with moderate requirements,’ he said, ‘lenses are aligned to one another at typical distances of 20µm to 50µm (air gap) and at height differences of around 10µm to 20µm with respect to a common optical axis. Naturally, the angles must be set precisely here. Such positioning normally is achieved using well-made mechanical systems, i.e. using classic processes like turning, milling, or grinding, depending on the material and geometry. If there are higher requirements on positioning accuracy, one must either design certain elements to be finely adjusted using micrometre screws or use techniques like ball chuck centring or adhesive bonding adjustment in the lens.’
A good resolution
Berliner Glas has developed a tool that can achieve a positioning accuracy of less than 1µm in order to position multiple elements simultaneously with high precision. The actuators used here are hexapods that allow adjustment on small assembly spaces in all six degrees of freedom. ‘When aligning in the micrometre range,’ said Beyer, ‘one must differentiate between the precision before and after the adhesive cures. Before hardening, precision of better than 250nm can be achieved, meaning quarter of a micrometre or half the wavelength of green light. Corresponding measurement equipment and optimised software algorithms are required to even be able to detect such values. If one uses, for example, image sensors to detect positioning, one can precisely determine the position of an edge at better than one tenth of a pixel using appropriate software. For 2µm pixels, the resolution is better than 200nm.’
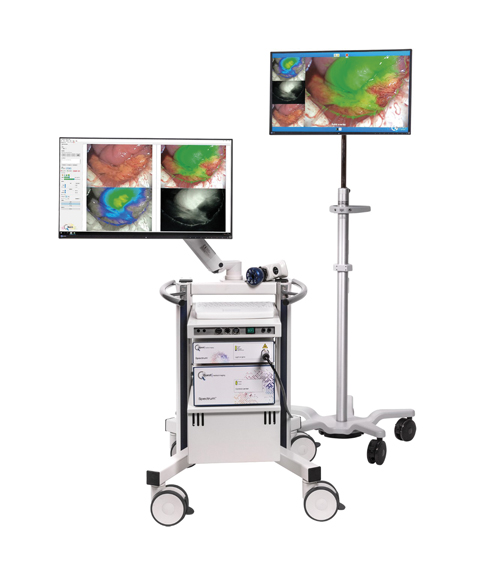
The Spectrum system includes a multispectral camera which images cancer cells and tissue differences not visible to the human eye. Credit: Quest Medical Imaging
In medical applications, there is a noticeable trend towards miniaturisation, so that smaller, more portable or table-top devices can be situated in theatres for easy access for surgeons. This trend often requires functional elements to be positioned in the single-digit micrometre range, said Beyer. ‘One could argue that insufficient precision could be offset through the use of software today,’ he said. ‘This is true, but only if there is no unknown information hidden in the system. Interpolating data points can only allow us to guess, not measure. An incorrect resolution, caused by poor alignment, always leads to more noise in the end, and thus to a higher uncertainty in the information.’
With the Berliner Glas adjustment platform the above and other electro-optical components can be precisely aligned for numerous visual procedures, including the kind of fluorescence imaging methods provided by companies such as Quest.
Beyer concluded: ‘By merging highly precise production processes for individual components and aligning them to one another with high precision, the result is a system that is capable of bringing out the maximum performance of a device.’


